Abstract
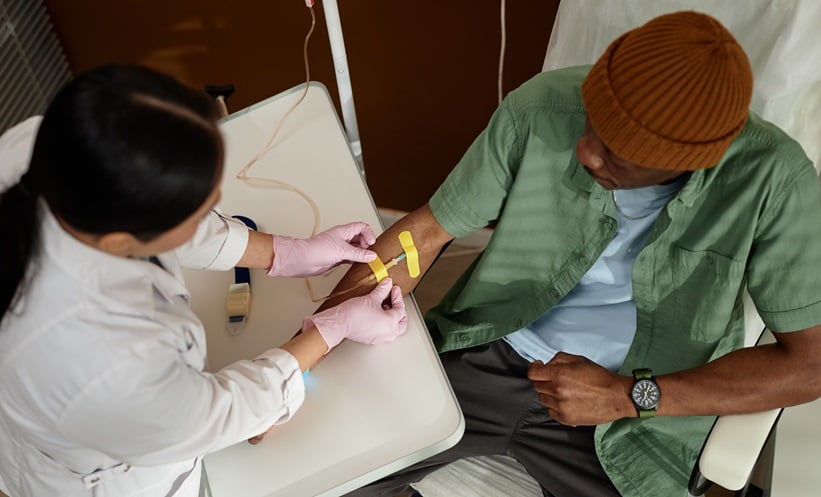
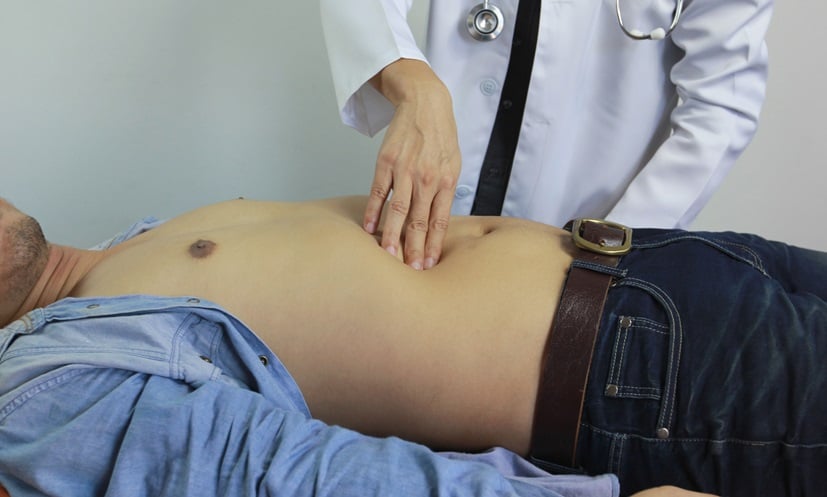
Alcoholic liver disease, a leading cause of morbidity, mortality, and cirrhosis, can range from simple steatosis to hepatocellular carcinoma. Multiple mechanisms such as oxidative stress, mitochondrial dysfunction, and alteration in gut-liver axis have been proposed for the pathogenesis of alcoholic liver disease. Based on different prognostic models, alcoholic hepatitis patients can be stratified into sub-groups and specific pharmacological therapy can be started. Alcohol abstinence has a clear cut mortality benefit and nutritional support is very important as most of the patients are malnourished and in a hypercatabolic state. Other than conventional glucocorticoids and pentoxifylline, newer agents and combination therapy can be used in severe alcoholic hepatitis in patients not responsive to conventional glucocorticoid therapy. Liver transplantation improves survival in advanced alcoholic cirrhosis and it can be an option in severe alcoholic hepatitis patients who are not responding to other medical therapies. Whether early transplantation can improve the survival compared with the conventional waiting period of 6 months is an active area of investigation. This is due to the fact that most of the disease-related mortality occurs in the first 2 months.
Please view the full content in the pdf above.